The Evidence Base
Based on Early Childhood Development Science
Recent scientific developments in understanding early brain and biological development tell us that the early years are important to all of us – the capacities and skills developed during this critical period become the basis of a prosperous society. The innovative approach of HealthySteps is designed based on scientific understandings of how early childhood development works and how it might be best supported.
A national evaluation and several subsequent site-level evaluations of HealthySteps demonstrate positive outcomes for children, families, and the providers that serve them. For more information, read this overview of our evaluation efforts.
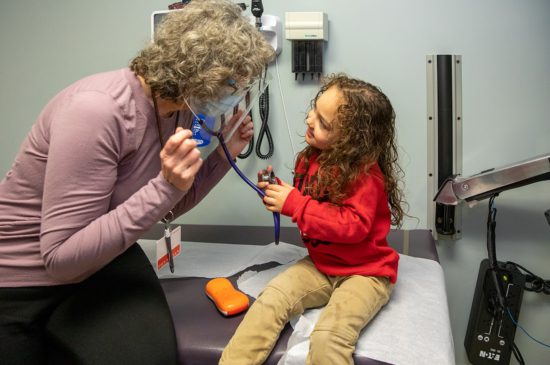
HealthySteps’ effectiveness was studied through a 15-site national evaluation conducted by the Johns Hopkins Bloomberg School of Public Health Women’s and Children’s Health Policy Center. HealthySteps was evaluated at six randomized and nine quasi-experimental sites. A diverse sample of 5,565 infants from 15 sites across the country was enrolled at birth and followed for three years. The study also included follow-up with children at 5½ years old. The model was shown to have significant benefits for children, families, and pediatric care in the United States. See the National Evaluation report and publications in the Journal of the American Medical Association and Pediatrics for more information.
When HealthySteps came to ZERO TO THREE in 2015, we partnered with an external evaluator to look under the hood and understand what was happening out there in the network. From these results, we codified the HealthySteps model to reflect best practices and the most recent research.
Key Outcomes
Child Impacts
HealthySteps improves child health and well-being by supporting perceptual, motor and physical development, strengthening early social-emotional development, and promoting timely and continued care.
Family Impacts
HealthySteps improves family health and supports a child’s early learning and overall well-being.
Practice and Provider Impacts
HealthySteps supports pediatric primary care practices to improve their patients’ experience and provider satisfaction while lowering health care costs.

Our Commitment to Growing the Evidence Base
We continue to build the HealthySteps evidence base to improve the lives of babies, toddlers, and their families. In 2017-2018 we partnered with Project Evident to develop a Strategic Evidence Plan with a roadmap for building our evidence base through 2021. Our Evaluation Advisory Group continuously informs our ongoing research efforts. We focus on assessing the implementation of the model and demonstrating key child, family, and provider outcomes.
The National Office collaborates with HealthySteps sites and other stakeholders to further develop the HealthySteps evidence base. To refine our model and drive continuous quality improvement, we launched the Outcome Pilots Study in partnership with James Bell Associates and MDRC in 2018. The study assesses our model’s influence on five outcomes important to healthy child development and family well-being.
We partner with other organizations and stakeholders on broader research initiatives such as an evaluation of the Get Ready Guilford Initiative that seeks to understand the collective impact of multiple evidence-based programs, including HealthySteps, at the community level.
Together with our partners and sites, we participate in several national research initiatives, including the HERO study led by the Harvard Center on the Developing Child and the JPB Research Network on Toxic Stress, and the Early Relational Health Measurement project led by the Center for the Study of Social Policy as part of the Pediatrics Supporting Parents initiative, to advance the broader field of early childhood development.
